NY Dems Pass Medical Debt Relief as Progressives Push to Expand Healthcare to Undocumented Residents
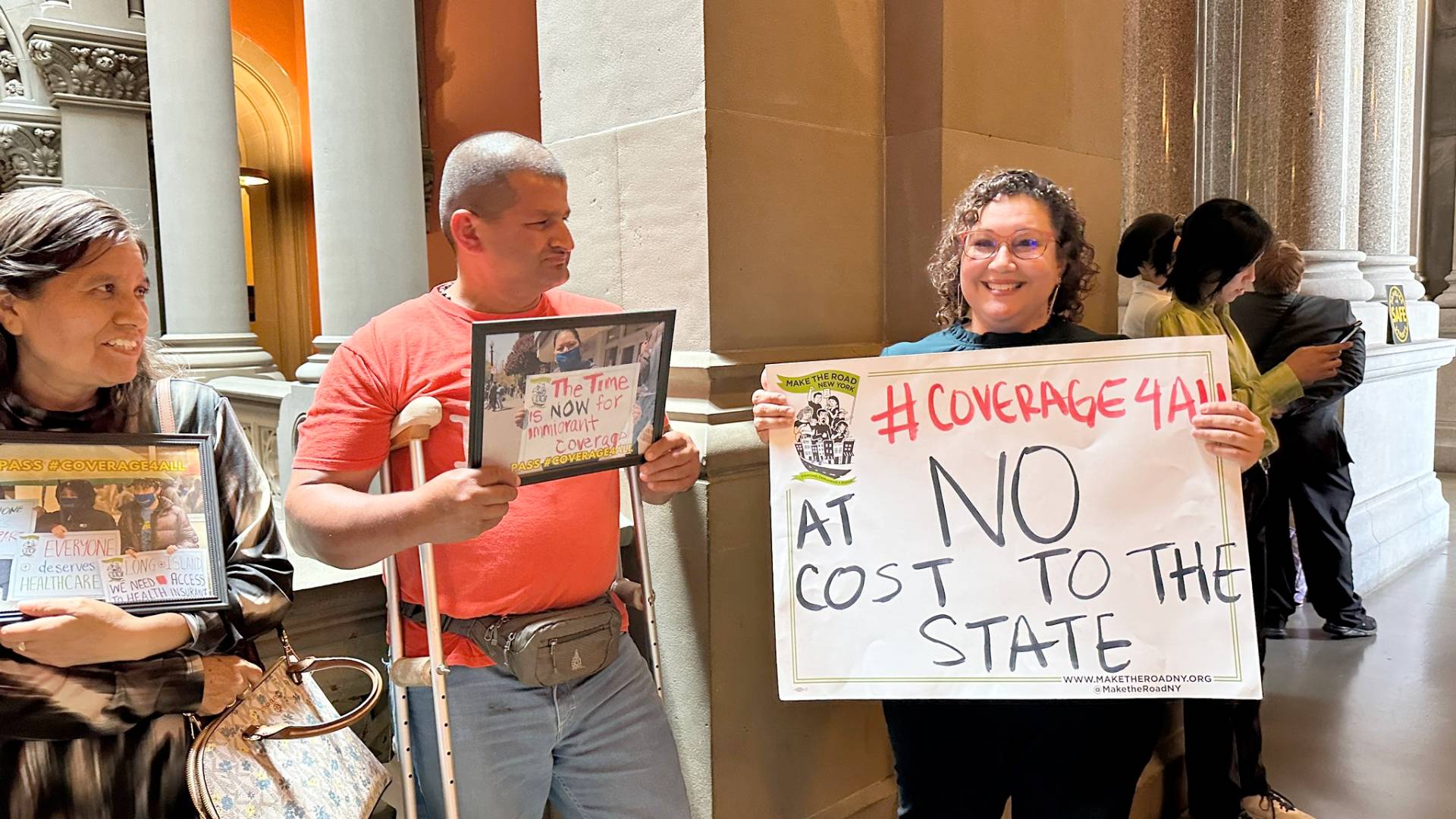
This is a rush transcript. Copy may not be in its final form.
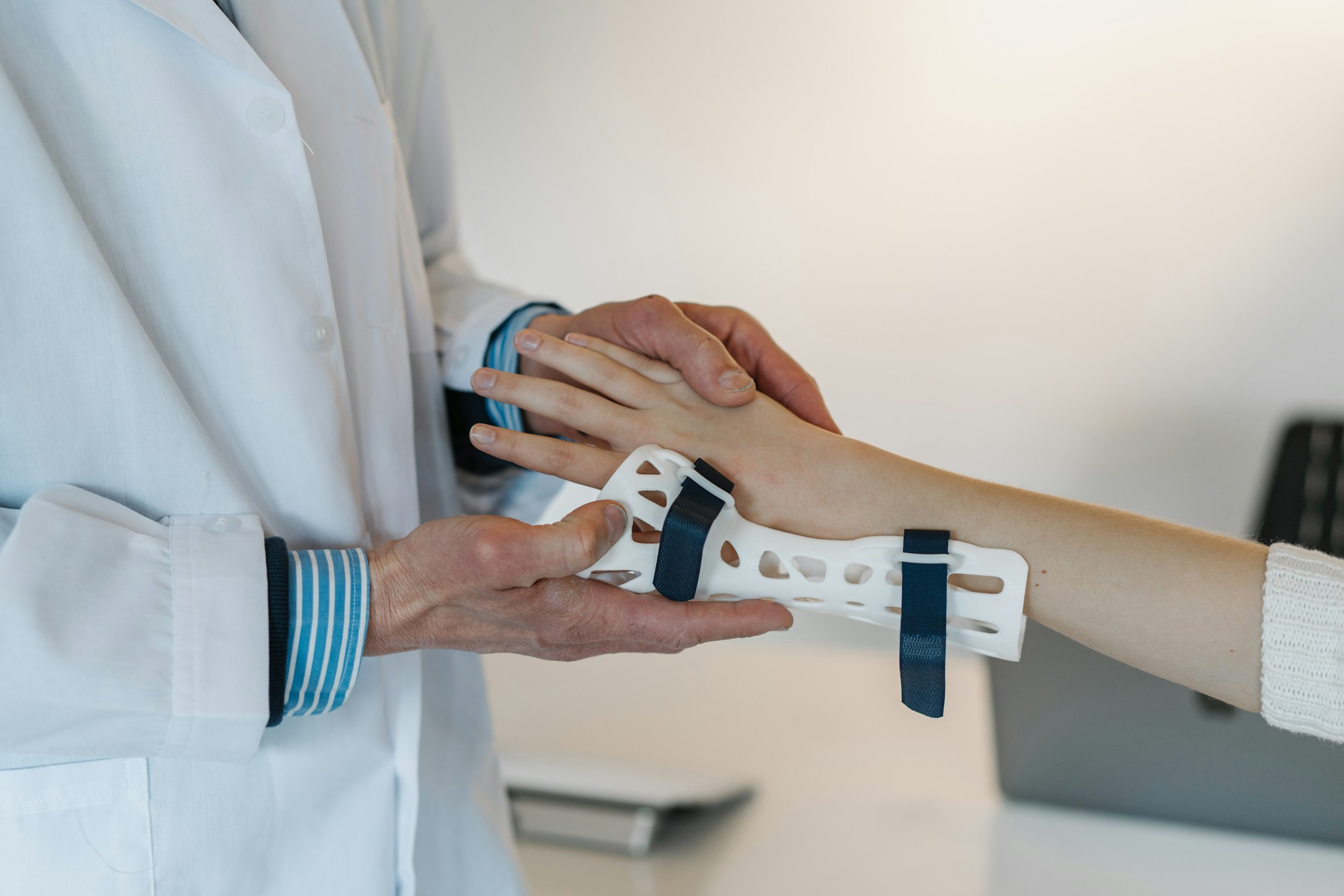
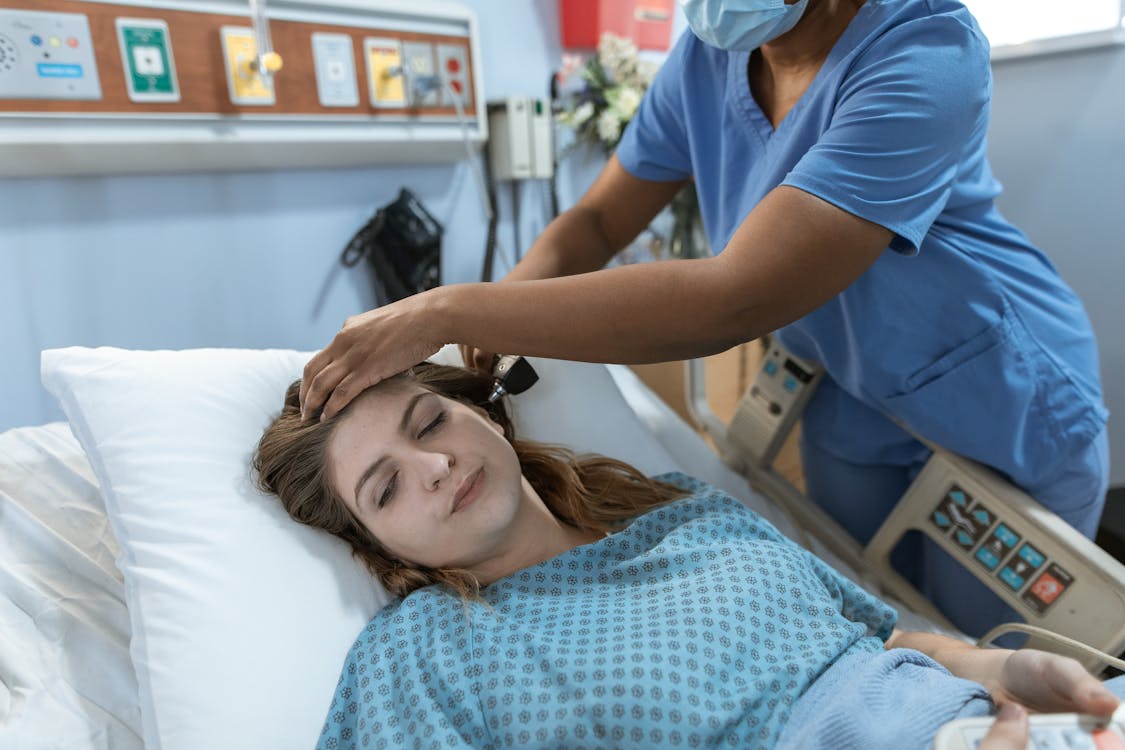
AMY GOODMAN: We begin today’s show here in New York, where the Democratic governor, Kathy Hochul, faces pressure to expand healthcare coverage for people regardless of their immigration status. Democrats hold supermajorities in both chambers of the New York state Legislature, and today is the second of a two-day special session where state Assembly members could vote to expand health coverage for thousands of people in a bill called Coverage for All, which would use a surplus of federal funds, allowing people who are undocumented to enroll in New York’s Essential Plan under the federal Affordable Care Act. Currently, over a quarter-million New Yorkers are excluded from Medicaid in the Essential Plan healthcare coverage due to their immigration status.
The measure is sponsored by New York Assemblymember Jessica González-Rojas, who negotiated with the governor to address cost concerns. But this week it was not included in a list of legislation to be considered in this final special session by Assembly Speaker Carl Heastie, prompting immigrant advocates to rally outside the Assembly as lawmakers returned for their session Tuesday.
This comes as Governor Hochul is set to sign a measure that did pass in the Assembly Tuesday and is celebrated by healthcare advocates because it would bar credit reporting agencies from collecting medical debt or including medical debt in a consumer’s credit report. A survey by the Community Service Society of New York found more than 40% of New Yorkers have paid a medical bill that may not have owed, out of fear of it being sent to collections. Meanwhile, about the same percentage said they had avoided getting healthcare they needed because of the cost.
For more, we’re joined by two guests. In a minute, we’ll speak with New York State Assemblymember Jessica González-Rojas, but first to Elisabeth Benjamin, vice president of Health Initiatives at the Community Service Society of New York and co-founder of Health Care for All New York campaign.
Elisabeth, welcome back to Democracy Now! Why don’t we start off with this medical debt victory that you’ve had in both houses of the New York Legislature, before we move on to the issue of immigrant healthcare? Talk about the medical debt bill that just passed by the Assembly, was already passed by the Democratic supermajority in the Senate.
ELISABETH BENJAMIN: Sure. Thank you for having me back on Democracy Now! It’s really exciting to be here again.
Well, 80 million Americans have medical debt. Medical debt is a severe problem for folks. You already outlined some of the issues, but I just want to point out that there are also profound racial disparities in medical debt. Twenty-eight percent of African American folks have medical debt versus 22% of white folks, and — pardon me, 22% of Latinx folks, and then 17% of white people have medical debt. So, that is a profound problem for people.
One of the ways that medical debt is experienced is, once you run into medical debt, fairly quickly, healthcare providers and their collection agents report you to the big three credit reporting bureaus. And you might think, “Well, at least they’re not suing,” or “What’s the big deal?” But it is a big deal. Credit reports are used for people to apply for jobs, for applying for apartments, for applying for a loan, for applying for a school loan. And so it really has profound ramifications. We were working with a guy that runs a tow truck business in Oneonta County. And he, basically, having had to go to SUNY Upstate Hospital, he ended up having a big $10,000 bill. It ruined his life. He lost his towing business. He could not get more loans to buy more tow trucks or to lease more tow trucks, and his business went under. This is what happens every single day to people by having medical debt reported on your credit report.
So, we’re really excited. Colorado, at first — I want to just give a big shoutout to the advocates in Colorado. But there’s been this movement around the country saying, “Well, wait a second. Why are we reporting medical debt in the first place?” It’s not like people are buying, you know, a new leather couch and racking up bills beyond their means. People go to get healthcare mostly out of emergencies or medical necessity. So, why are we reporting this in the first place?
But not only that, when they started analyzing — when the experts analyzed what’s on credit reports, they found that they were rife with errors in the area of medical debt. And we all know why, right? The insurance company doesn’t bill properly — I mean, the healthcare provider doesn’t bill the insurance properly. The code is wrong. The insurance company accidentally rejects it, or intentionally rejects it — who knows? There’s this whole back-and-forth, this dance between — you know, in our really weird patchwork healthcare system, it’s not that insurance company’s responsibility, it’s a different insurance company’s responsibility. Who knows? But anyways, the medical debt that is on people’s credit reports is — more often than not, shouldn’t be there in the first place.
Then, on top of it all, study after study has shown that when lenders look at credit reports and they analyze medical debt, that is not predictive of whether someone is a good lending risk or not. So, what’s the point of having incorrect and nonutility — their no utility medical debt on a credit report in the first place?
Which is why, thanks to the Assembly and the Senate, you know, 740,000 New Yorkers, moving forward, will no longer have medical debt on their credit reports. And we couldn’t be more delighted here in New York. And a big shoutout again to our friends in Colorado, who did it first. We’re second. But we know many other states are considering this same piece of legislation, now that the federal Consumer Financial Protection Bureau said it was OK to pass this on the state level.
JUAN GONZÁLEZ: Elisabeth, I wanted to ask you about another health-related issue, the issue of Medicaid eligibility. There was a huge increase during the pandemic in the number of people who were able to use Medicaid, who had lost their jobs. But now, starting in April, this past April, there’s now a question — a mandate to reevaluate eligibility. What’s going to be the impact on the Medicaid enrollment as a result of this?
ELISABETH BENJAMIN: Yeah, so, what happened is, during the pandemic, the federal government — I believe first under the Trump administration and then in the Biden administration — said, “OK, we’re not going to force people to prove their life every year in order to maintain Medicaid coverage,” and also, in New York state, Essential Plan coverage. “We’re going to just say” — you know, people’s incomes rarely change, fluctuate during the year anyway. “We’re just going to roll them over.” And so, that rolling over of everybody’s Medicaid eligibility and public coverage eligibility happened for about three years.
You know, as we all know, COVID has been declared eliminated, or at least over. And so, on May 11th, the administration said, “OK, we’re going to stop requiring states to continue that coverage, you know, renewal, automatic renewal. And we’re going to require the states, over the next 14 months, to take a look at their public insurance rolls and sort of slow” — and in New York state, for example, we’re doing it batch by batch, month by month. We’re having everybody come in and renew their coverage. The very sad thing is that some states are not like New York, and they just kind of are just bombing through these renewals and just kind of, it seems — it would appear that there is, you know, a huge volume in disenrollments.
We’re lucky, again, in New York. We have a really different approach. It’s an all-hands-on-deck approach. We were very lucky that we went to eight funders. My own organization went to eight funders, and we have this great consortium of New York-based funders who are giving microgrants through the Community Service Society of New York to over 36 local community-based organizations, covering nearly every single county of New York, to kind of do boots-on-the-ground outreach, local media buys, to kind of tell people, “Hey, come in. Renew your coverage. Let’s try to keep every single person who’s eligible on coverage over the next 14 months.”
And so far, it seems to be going pretty well in New York, but not so well in other states. And I think it just shows the different approach to whether, you know, people really — state officials really value the importance of people having coverage, which we think is so fundamental to people being able to have effective and productive and healthy lives.
AMY GOODMAN: Elisabeht, I wanted to play a clip from We the Patients New York, which has spoken to many people struggling with medical debt. This is Anthony Calafiura’s story.
ANTHONY CALAFIURA: So, slightly over a year ago from now, I was committed to the psych ward after a failed suicide attempt. I was there for 14 days. It genuinely helped me, until I received my bill afterwards. But, thankfully, I was under my estranged father’s insurance. But even then and currently today, I am over $2,000 in debt, and my mother has refused to help me pay, so I have essentially been forced to kind of figure out this whole situation by myself.
And when I was committed, I was 17. So, after I got released, when I tried calling, like, the hospitals, there wasn’t much I could do, because I was still a minor. And it just felt like a circle, and I never really got, like, actual advice on what to do.
Now that I’m 18, it’s been like six months since I’ve been released, so all my debt has been transferred to the debt collection agency. Nobody around me really knows what to do. And this whole situation has just been causing me so much stress. It’s like every time I check my mail, every time I receive an 866 call, which now I know is the debt collection agency’s number, every time I see a minor text, I’m just reminded of how much debt I’m in, and it just makes me really anxious, and it’s been really not good for my mental health, which is why I’m even in debt in the first place, was to get better.
I think there should be a law changed within the medical system. I think in schools they should teach you about how insurance works, even how to manage debt.
For the most part, I’ve just felt really alone, even when there are 23 million Americans in debt, which is, essentially, one in 10 Americans.
In general, the U.S. healthcare system, people shouldn’t have to go into debt, with like little knowledge on what to do after, just to get the medical care that they need. People also just shouldn’t be afraid and resistant to go in to the doctors in fear of the bill that they’re going to receive after.
AMY GOODMAN: Just before we go to the state assemblymember, Elisabeth, the significance of his age on the issue of medical debt?
ELISABETH BENJAMIN: Yeah, it’s ridiculous. You know, if his mother had disavowed him, he would have been considered an emancipated minor. He would have been eligible for Medicaid or Child Health Plus. That hospital or mental health facility never should have put him into collections. You know, all these facilities in New York collect millions of dollars in indigent care pool funds that could have been applied to his case. There’s just no good reason for him to have been put into collections, and it’s actually heartbreaking. And it’s why we have these things like my agency runs called the Consumer Assistance Program, that was funded under the Affordable Care Act for the first year and then never funded again, basically, over Republican opposition not to fund these consumer assistance programs that could help people like him, who was completely eligible for coverage at the time. It’s just heartbreaking.
AMY GOODMAN: I want to bring, in addition to Elisabeth Benjamin, Jessica González-Rojas, New York state assemblymember representing the 34th District in Queens. Her op-ed in El Diario Tuesday was headlined “The Assembly Can Make History by Passing Health Coverage for All.” Assemblymember, can you start off by talking about the significance of what it would mean? I mean, we’re talking about a Democratic supermajority in the Assembly. Already, the Democratic supermajority in the New York state Senate passed this. Why hasn’t this bill been brought to the House floor? And talk about exactly what it is.
ASSEMBLYMEMBER JESSICA GONZÁLEZ-ROJAS: So, first off, thanks for having me, and thanks for talking about this important topic.
As I mention in my op-ed, this is an opportunity for us to make history. This is a moment where we have a bill that will direct the commissioner of health to submit a federal waiver, the 1332 waiver, that would allow for us to use federal surplus dollars in order to cover a population in our state, our New York state undocumented residents, who utilize healthcare. And currently we’re spending our emergency Medicaid dollars to get their healthcare. But what this bill would do is allow us to use federal surplus money to allow them to enroll in our New York state health insurance plan, called the Essential Plan. This is groundbreaking, because we have an opportunity to utilize surplus federal dollars.
Washington state got this waiver approved. Colorado got this waiver approved. There is, as you mentioned, no reason why we shouldn’t be able to move forward. It passed in the Senate. We are in active conversations with our colleagues in the Assembly. We are in a special session right now. And I’m still optimistic that we can push this through, but we really just have today.
JUAN GONZÁLEZ: And, Assemblywoman, what does Governor Hochul say about this? Why is she opposing it? I understand she claims it’s going to cost $2 billion to $3 billion annually. But your perspective is that it will actually, in the long term, save money to the state. Could you talk about the differences there?
ASSEMBLYMEMBER JESSICA GONZÁLEZ-ROJAS: Absolutely. This will not cost the state any money, and, in fact, will save the state about half a billion dollars in emergency Medicaid costs that we bear as a state each year for the cost of care for undocumented people. And again, these are folks that are in dire emergency and are ending up in the emergency room. That is not quality healthcare. We can instead submit this federal waiver to use federal dollars at no cost to the state — and I want to be incredibly clear: no cost to the state — to allow folks to enroll in our New York state Essential Plan. Again, these two states have done it.
What we’ve added to the bill to make sure to guard against any concerns around costs is allow the commissioner to create guard rails. They can cap the program. They could limit it to a certain federal poverty level. They could put a dollar amount. But again, these are the use of federal dollars. We garner a surplus every year through a statute in the Affordable Care Act, and we are pretty much guaranteed about $2 billion of surplus funds every single year. And we’ve seen that since our program started in 2015. And this would just expand eligibility for those people who are New Yorkers, who are residents of New York, and would otherwise qualify except for the immigration status. So, this would allow those folks to enroll in health insurance, be much healthier. They’re a low-cost community. Our immigrants are actually a very healthy community. So, it would actually bring down the costs for everyone to administer the program, and perhaps can even garner additional surplus funds.
JUAN GONZÁLEZ: And you’ve mentioned these federal surplus funds. What are they exactly? And where are they hiding in the budget?
ASSEMBLYMEMBER JESSICA GONZÁLEZ-ROJAS: So, they are money that when we created our New York state Essential Plan back in 2015, we had to submit a waiver that said that we would create our own state plan, and the federal government will reimburse the state 95% of what they would spend, because right now the ACA requires a federal marketplace. So, because we created our own state plan, we have this agreement to get reimbursed like credits up to 95% of what the federal government would have spent. Well, we’re way under the cost of what the federal government would spend, so we get reimbursed, but we have actually accumulated about $2 billion per year since the program started in 2015. And right now we’re sitting on about, you know, $11 billion trust fund.
We cannot use that trust fund to cover the undocumented communities. We have to submit the waiver that’s directed in my bill, called Coverage for All, in order to be able to use future surplus funds. But again, we’ve garnered these funds since our program started, our Essential Plan program in the state, and we anticipate that we’ll continue to bring in those surplus funds. And that pot of money can be used — and we got a letter from the federal Centers for Medicaid and Medicare Services that said, “Yes, you can use the surplus funds to cover undocumented communities.” Again, two other states have gotten this approval. We should be next.
AMY GOODMAN: Assemblymember González-Rojas, not that I comment on women’s clothes who are our guests, but I can’t help but notice that you’re wearing a necklace that says “daughter of an immigrant.”
ASSEMBLYMEMBER JESSICA GONZÁLEZ-ROJAS: Yes.
AMY GOODMAN: If you can talk about the significance of what this means, and also the support that your bill has gotten from a hundred unions, health plan providers, community organizations, that have signed a letter to the Assembly speaker, Heastie, urging the passage of this bill?
ASSEMBLYMEMBER JESSICA GONZÁLEZ-ROJAS: Yeah, this — I mean, personally, as a daughter of an immigrant, my father is from this teeny tiny country in South America called Paraguay. He came in the ’60s, and, you know, he came in with legal — as a legal permanent resident. But I represent a district in western Queens — Jackson Heights, East Elmhurst, Corona, Woodside, Astoria — that has such a large immigrant community and many, many who are undocumented. So, personally, as a daughter of an immigrant and someone who represents a district that has a vibrant — a vibrant immigrant population, many who are undocumented, many who were those essential workers who ensured that we survived during this pandemic — they were out there, you know, providing those essential services, deliveries. They were street vendors. They were people at the frontlines. They deserve healthcare.
And as was mentioned, we had tremendous support. I mean, we have everyone from the Business Council to the Greater New York Hospital Association to countless unions, the healthcare union, DC 37, RWDSU. We have advocacy organizations. We have tremendous support. The previous health commissioner of New York state, Mary Bassett, submitted comments in support of expanding coverage for our undocumented community under this fed waiver.
So, we don’t understand why the governor is resistant. She said that she would work with the federal government last year, because we were very close to getting this done last year. She said she’d work with the federal government. We’ve been working with the federal government. Then she said she wanted a letter of guidance from the federal government. We got that letter of guidance on June 6th. So, that sort of fast-tracked the bill. We were very fortunate to get our Senate sponsor, Senator Gustavo Rivera, who is a big fan of this show. He was able to move the bill in the Senate. So, again, there’s no reason why we shouldn’t get this done in the Assembly. It’s really a win-win-win for the state, for our communities, with the tremendous amount of diverse support that’s behind this.
JUAN GONZÁLEZ: Yeah, I wanted to bring in Elisabeth Benjamin again, just a quick thing, because we don’t have much time. But, Elisabeth, could you give us a quick sense of what has been happening with the thousands of asylum seekers that have been sent here by Republicans and governors in Texas and Florida? What’s their situation in terms of healthcare access?
ELISABETH BENJAMIN: Well, they’re actually already eligible. They’re lawfully present because they’ve, you know, registered themselves at the border. They’ve applied for asylum.
So, this surplus is really for our longtime essential workers, who work their — you know, worked their fingers to the bones throughout the pandemic, and really for the longtime immigrant population who’s already here. Many of them, as Assemblywoman González-Rojas said, are already availing themselves of the emergency Medicaid program, at great cost to the state of New York and the federal government. We would be saving, combined, a billion dollars a year, if we just went for this Coverage for All bill and had the federal surplus funds be used instead, so people could have comprehensive coverage for all of their regular preventive health — vaccinations, everything, they could then get, as opposed to this episodic, willy-nilly, high-cost emergency room care.
So, I think Assemblywoman González-Rojas just nailed it. The time is now. We must do this. Our waiver is already pending before the federal government. All we need to do is amend it to include immigrants. The math is done. We’re ready, Freddy. Let’s get this done.
AMY GOODMAN: Elisabeth Benjamin, vice president of Health Initiatives at the Community Service Society of New York, and Jessica González-Rojas, New York state assemblymember, thanks so much for joining us.
Next up, we look at the “Minnesota Miracle,” at Minnesota’s Democratic supermajority and governor, who have just enacted sweeping progressive reforms. And we’ll go to Minneapolis as the Justice Department concludes police disproportionately targeted Black and Native American people. Stay with us.