Much more health care use is not the solution to our conditions

- Mohammad S Razai, NIHR in-observe fellow in most important care,
- Pippa Oakeshott, professor of standard follow
Tens of millions of people are ready to accessibility care in a method under huge pressure. Extensive waits can direct to poorer outcomes and exacerbate the struggling of individuals trying to get treatment, a little something that we really should not forget about. Nevertheless, we have to also admit that more healthcare does not necessarily mean better health and fitness. It is significantly obvious that health-related overuse can have detrimental consequences on wellness and wellbeing.1
Over the earlier couple of many years in industrialised nations around the world, diagnostic resources, surgical techniques, and pharmacological treatment options have turn out to be superior and extra available. There has also been sustained development in need for healthcare services, which is projected to improve further more.2 In English major treatment, despite the falling range of common practitioners, NHS England experiences an enhance of 35 million appointments in the 12 months ending July 2022 when compared with the 12 months ending July 2019, from 310 million to 345 million.3 Even further, details present that 7 million individuals in England are “awaiting clinic treatment method,” a determine that is envisioned to rise.4 The soaring demand from customers for professional medical treatment is partly brought on by an ageing inhabitants and an maximize in serious ailments exacerbated by the current pandemic.5 Even so, this is not the complete story. The unrealistic anticipations of fashionable overall health nervous societies6 and the misplaced trust in the guarantees of modern day drugs are also drivers of health-related overuse and unnecessary treatment.7
Even with comparatively much better access to clinical treatment and an exponential rise in biomedical study funding,8 existence expectancy in nations around the world this kind of as the United Kingdom and United States has declined.9 Dissatisfaction with present day health care is rife,1011 and gratification with the NHS throughout the socioeconomic spectrum, age, gender, and political celebration affiliation is at the most affordable level (36%) considering the fact that 1997.11
Furthermore, there is developing evidence of harm from health care interventions. For case in point, one research identified that people at large danger of coronary heart failure and cardiac arrest admitted through a national cardiology assembly, when 1000’s of cardiologists have been absent, had a substantially reduced 30 working day mortality charge than comparable clients admitted in the months ahead of and soon after the meeting.12 The study shows that it is achievable that “more interventions in significant hazard people qualified prospects to increased mortality.”13 Around the previous 20 several years, the quantity of high risk people undergoing surgery in the NHS has doubled, making up about 450 000 of the three million persons operated on each year.14 A fifth die in just a 12 months, earning up 4 fifths of put up-surgical deaths.14 The World Health Corporation phone calls health care relevant adverse functions 1 of the world’s 10 main triggers of dying and incapacity. In higher profits nations around the world, a single in 10 individuals is harmed whilst acquiring medical center care.15 The condition is significantly worse in very low and center earnings nations around the world, the place 2.6 million fatalities happen while patients are obtaining care.15
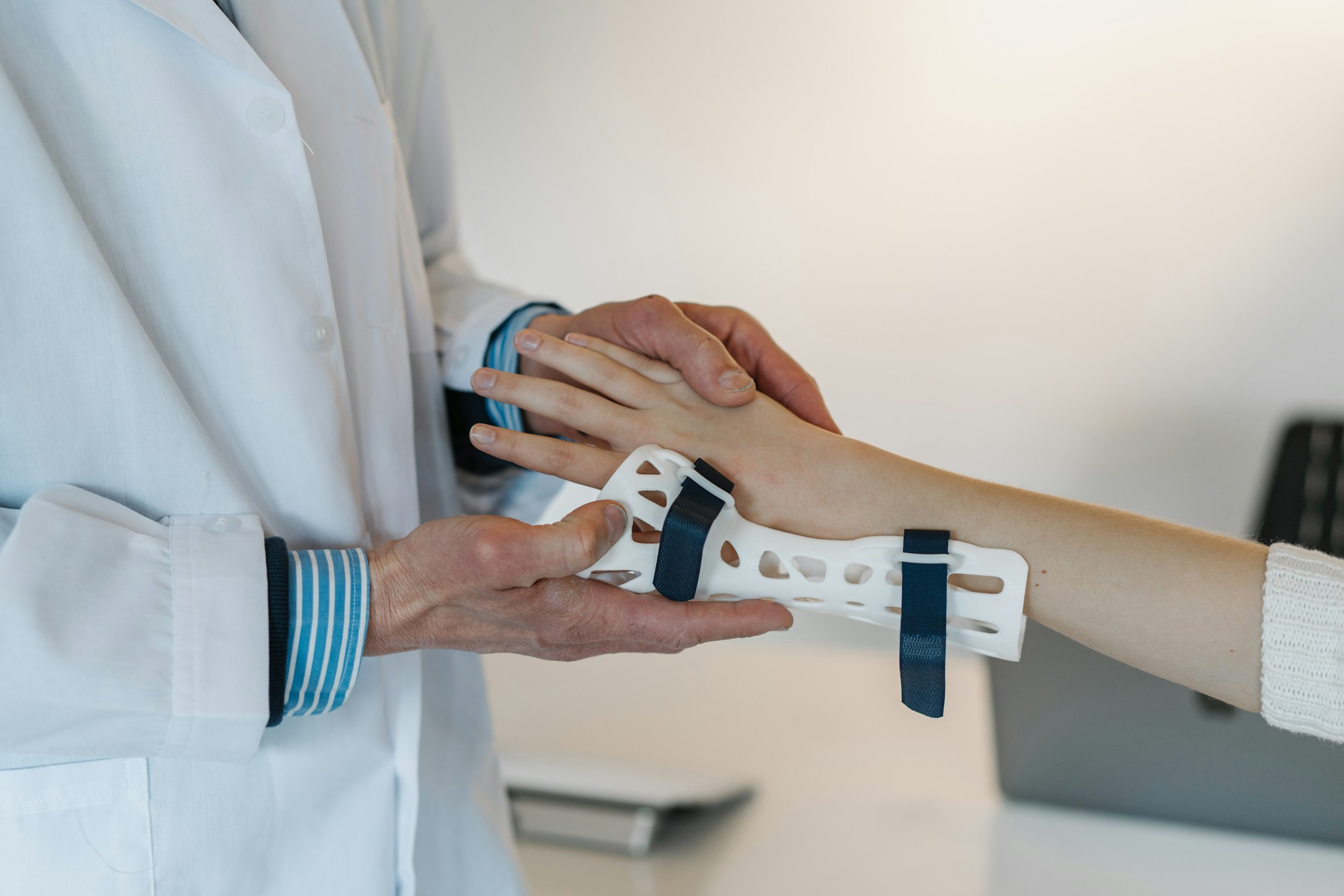
As key treatment clinicians, we commit sizeable time reassuring the anxious well—healthy persons worried that they have concealed illnesses that need to be diagnosed and addressed. Some men and women are nervous that any symptom, even if minimal, is often a harbinger of critical fundamental pathology. The needs of these individuals for reassurance account for numerous unwanted and inappropriate diagnostic referrals and overtreatment.1617 It has been continuously shown that around tests will cause false constructive outcomes and overdiagnosis. On the other hand, adverse take a look at effects may well fall short to reassure men and women.1 A minimal symptom that would have improved can spiral into an unstoppable chain of invasive investigations, professional medical solutions, and opportunity surgeries. For instance, a lot of folks with unpleasant knees request a magnetic resonance impression scan. But a torn cartilage observed on this sort of a scan may well not trigger any pain, the soreness may perhaps not be connected to the tear, and the final result generally does not influence management. A randomised managed trial confirmed that the end result of arthroscopic meniscectomy was no much better than just after a sham surgical process.18
Also, lots of people today appear to us with slight conditions that do not want our abilities or information. They would have accomplished greater to request a wise buddy or family member or seek the advice of the NHS internet websites. Even for quite a few individuals with continual disorders (normally older populations), we might have arrived at the conclude of what biomedicine can give to reduce their suffering.
Abraham Maslow is extensively credited for declaring, “If the only tool you have is a hammer, you are likely to see each and every trouble as a nail.” It is not surprising, as a result, if someone will come to a health practitioner with a dilemma, that it will possible become a healthcare just one by default.
At current, several health and fitness methods are at a breaking place, and the present-day problem is not sustainable. The NHS is beneath massive tension, with many individuals in need to have of treatment, but unable to acquire it for the reason that of extensive waiting around lists and more than stuffed unexpected emergency departments. So, what wants to be finished? We ought to initial acknowledge that socioeconomic determinants largely form human wellbeing, and health care plays a comparatively minor job. Smart community health actions could assistance, but even the finest healthcare can not make us considerably more healthy. We need to concentrate on reducing socioeconomic inequalities as the main driver of ill wellbeing. Next, we are inquiring biomedical science to solve intractable human illnesses, such as outdated age, which it can’t do. Use of healthcare increases with age, and most means are devoted in the direction of the finish of lifetime, usually prolonging person struggling at a fantastic charge to modern society.719 As Seamus O’Mahony writes: “We are dealing with, and around dealing with, but not therapeutic.”7
Finally, the unquestioned mantra about far more access to health care is unhelpful and encourages a lot more intake and well being anxiety. There is a distinct will need for interdisciplinary lateral wondering that moves from concentrating exclusively on biomedical science and professional medical hyper-specialism to other expertise domains, including social science and humanities. There will often be a area and a need to have for health care, but we need to shift to a re-imagined environment with a radically unique conception of health and fitness and sickness.
Footnotes
-
Competing pursuits: none declared
-
Provenance and peer evaluation: commissioned, not peer reviewed
-
MSR is supported by NIHR as in-observe fellow. The sights expressed are people of the authors and not automatically those of the NHS, the NIHR, or the Department of Health and Social Treatment.