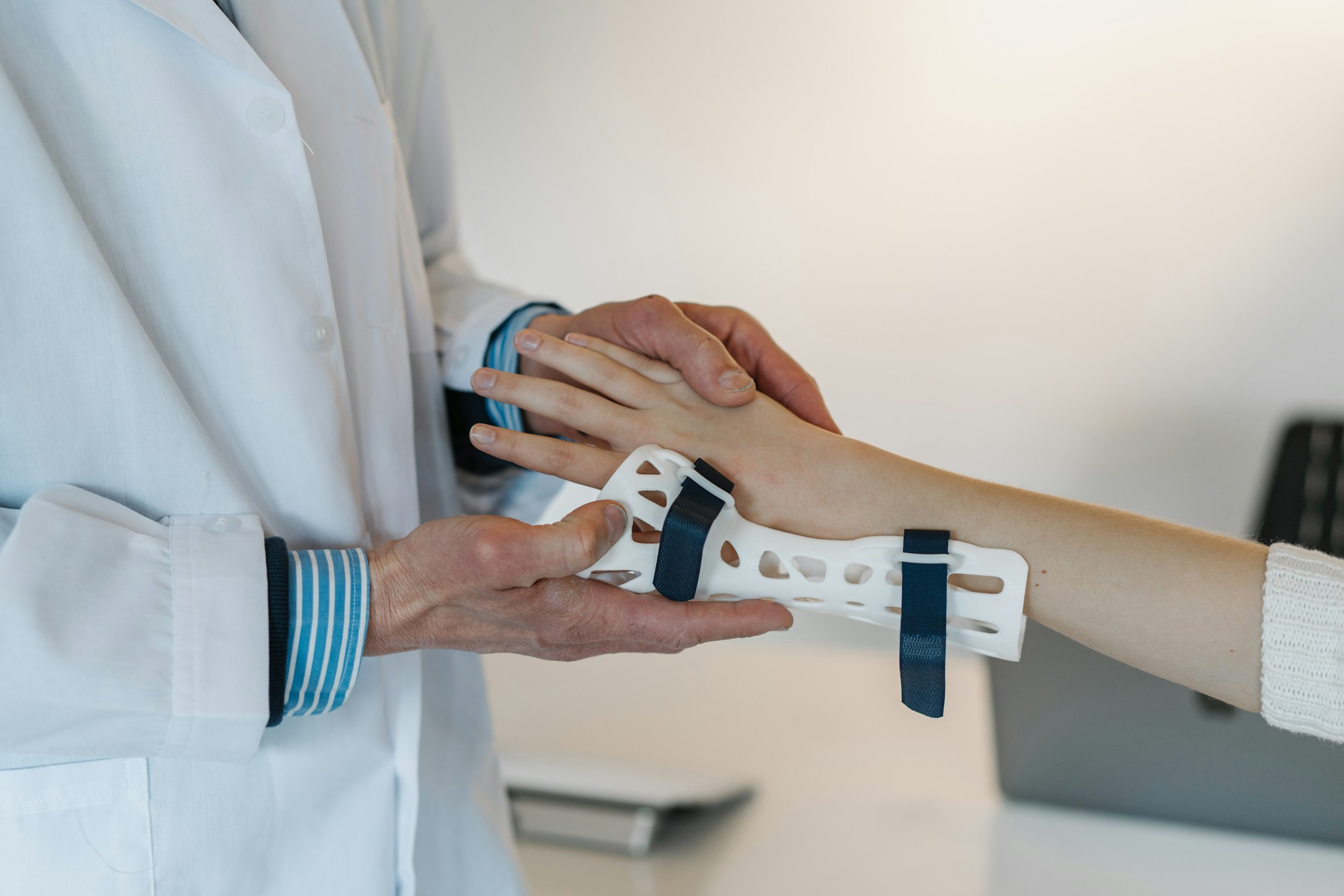
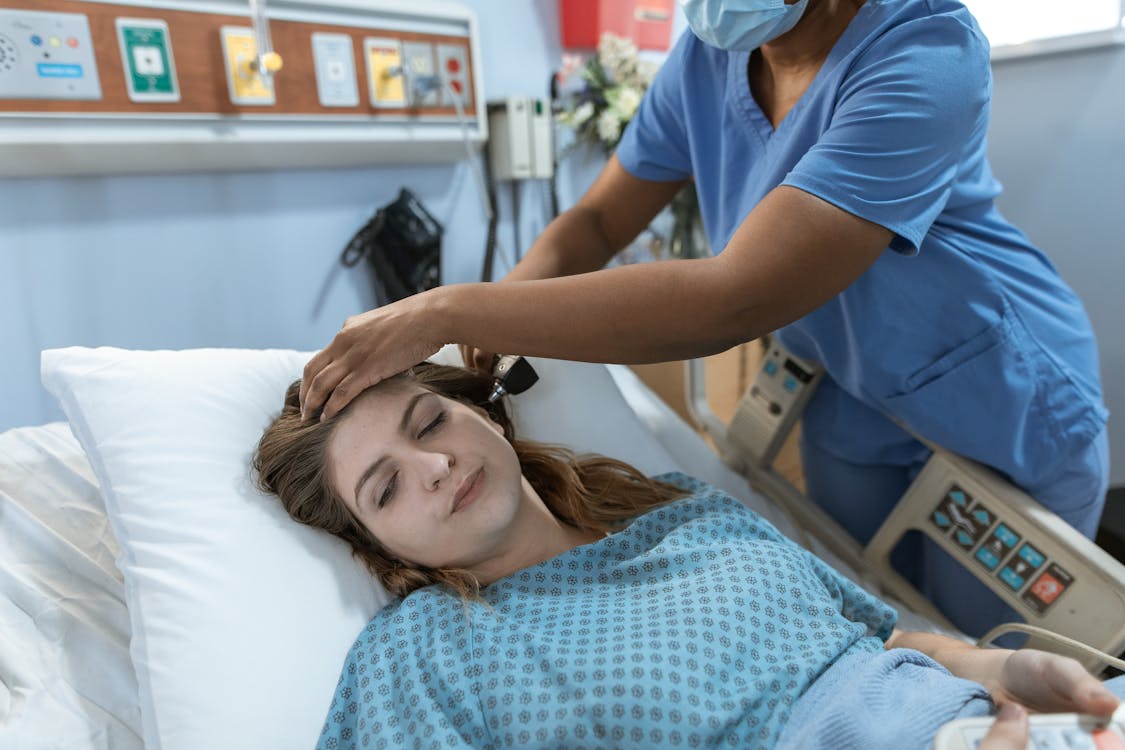
How Can We Boost Professional medical Treatment for Homeless Individuals?

Making belief, making sure continuity of treatment, and carrying out no hurt are critical tenets to increasing health care for homeless or “unhoused” people today, mentioned industry experts through an online briefing hosted by the Alliance for Well being Policy on Wednesday.
“Believe in is a massive deal” amid homeless people, explained David Peery, JD, co-chair of the Countrywide Shopper Advisory Board and Countrywide Health and fitness Treatment for the Homeless Council, who himself spent time dwelling on the streets.
Men and women who have been dwelling on the streets are equally emotionally and physically traumatized by the expertise, and they normally see the very establishments and experts that other people inherently rely on — including police and medical practitioners — as predators, Peery stated.
One reason for that distrust may be the criminalization of homelessness, or the interference of “daily life-sustaining activities” that folks who are homeless have interaction in — sleeping, feeding on, tenting, asking for income — by routines such as “sweeps” of encampments and prohibiting panhandling.
Peery illustrated with illustrations from Miami how criminalizing homelessness can have a considerable effects on wellness.
“We have documented circumstances of a girl likely into convulsions on the avenue simply because her medicine had been thrown absent by city staff just several hours earlier, and … of folks who are disabled, who have experienced their individual walkers and wheelchairs … thrown away,” he explained.
In other elements of the region, many years of outreach and a patient-centered approach have helped construct rely on with individuals in the homeless local community.
Road Medicine
About 75% of people today residing on the streets of Boston have been vaccinated from COVID-19, stated Jim O’Connell, MD, president and founder of Boston Health Care for the Homeless System (BHCHP) and assistant professor of medicine at Harvard Clinical University.
He claimed there was absolutely nothing magical about Boston’s outreach the vaccines had been recognized by individuals dwelling on the streets simply mainly because they have been offered by people today who experienced recognised them for several years.
In the early 1980s, the city of Boston obtained a grant from the Robert Wood Johnson Basis to make a healthcare system for the homeless. A stipulation of the grant was that the homeless men and women needed to be involved as stakeholders in the scheduling of the system.
People residing on the avenue stressed the importance of continuity of treatment, telling physicians at the time, “We want you to do this as your profession and not as a thing you just do as a temporary matter that you move on [from],” O’Connell stated.
Of the approximately 40 medical professionals at the moment working in the BHCHP, most started as inhabitants or professional medical learners and stayed. O’Connell, who experienced himself prepared to work for a year and then transfer on to a fellowship in oncology, also stayed.
Just about every medical professional will work alongside a nurse practitioner or a health practitioner assistant, and currently also with psychiatrists and recovery coaches, all serving the exact same panel of clients. All suppliers assembly patients out on the road are needed to be credentialed in a single of the two main hospitals — yet another layer serving to to encourage continuity in patient treatment, as this reduces the want to refer to one more clinician in the medical center.
Also, because individuals questioned for treatment groups that achieved them where they have been, the shipping model concerned doctors keeping clinic in the clinic in the course of daytime hours — as shelters are normally closed throughout the daytime hours — and then in shelters and streets in the afternoons and evenings.
For O’Connell and other physicians, assembly patients where by they have been also intended participating in overnight journey-alongs with peers (individuals with lived experience of homelessness) in a van providing unhoused people today soup, sandwiches, and blankets. Although distributing these products, O’Connell would nonchalantly say to whomever he achieved, “By the way, if you will need something, I am a physician.”
That “back doorway” tended to function both equally as a signifies of providing care and constructing rely on, in accordance to him.
Healthcare Respites
A person of the challenges hospitals all over the place experience day-to-day facilities about discharging homeless people just after their care is complete.
“We have documented occasions in which an unique who was discharged on to the avenue has died, various instances … pretty practically, just both across the road or ideal down the block from the clinic,” Peery said.
He mentioned that guidelines and regulations advise in opposition to, and in some circumstances penalize, hospitals for discharging unhoused people today who are “not sick ample to be maintained in the small-phrase acute-care placing, but are way also sick to take treatment of on their own on the streets.” Despite scenario managers’ and discharge planners’ most effective endeavours to uncover websites of transitional treatment, it continue to transpires that homeless people are launched with nowhere to go.
Just one answer has been healthcare respites, which go over and above only serving as a transitional area and provide a number of gains, discussed Barbara DiPietro, PhD, senior director of coverage at the National Health and fitness Treatment for the Homeless Council.
O’Connell experienced released the initially healthcare respite in the early 1990s. The earliest packages functioned primarily as AIDS units in the course of the peak of the HIV epidemic, he noted.
These days, health care respites present a bridge for people to principal treatment and behavioral health and fitness sources, delivering time for clinicians to equally develop a treatment plan and to discover to far better control patients’ prescription drugs for any long-term health conditions.
As a result, these services have been linked to far better outcomes for individuals, shorter hospitalizations, and reduced readmission rates, which will save expenses all through the health care method, DiPietro claimed.
Peery pointed out that healthcare specialists in Miami are searching to replicate this model.
Expanding Accessibility to Treatment, Decreasing Harm, Housing
Panelists touted Medicaid growth as another way to help and enrich treatment for unhoused people today.
“The failure to expand Medicaid is not only a ethical failure, I would contend, but also a general public health failure,” reported Peery who life in Florida, just one of 12 states that has still to extend Medicaid eligibility to grownups below age 65 whose earnings is at or underneath 138% of the federal poverty stage.
In addition to reliable continual care and creating relationships and Medicaid eligibility, harm reduction is essential to aiding offer efficient care for people living on the road, panelists explained.
Via packages aimed at lowering a person’s hazard of drug overdose or obtaining HIV and hepatitis C, harm reduction can entail delivering homeless folks with syringe trade companies, fentanyl check strips, and naloxone (Narcan).
There are also other improvements like safe and sound use web-site or secure injection facilities that “decrease the hurt behaviors, and maintain folks alive so that we have yet another day in which we can do the outreach needed to get them linked to treatment,” DiPietro said.
One particular principle that can get lost but maybe transcends all of the other products is the basic strategy that “secure housing is important for secure overall health,” DiPietro claimed.
Analysis indicates that individuals who are homeless have significantly bigger rates of diabetic issues, hypertension, and other chronic challenges than the standard community. In addition, very poor well being can cause homelessness, as medical credit card debt can guide an person to lose a residence and obtain to treatment.
“So when we say ‘housing is health care,’ that’s wherever we’re coming from,” DiPietro reported. “Nothing that we do with health care providers performs as very well if somebody goes again to the shelter or underneath the bridge or to the encampment.”

![author['full_name']](https://clf1.medpagetoday.com/media/images/author/shannonFirth_188.jpg)