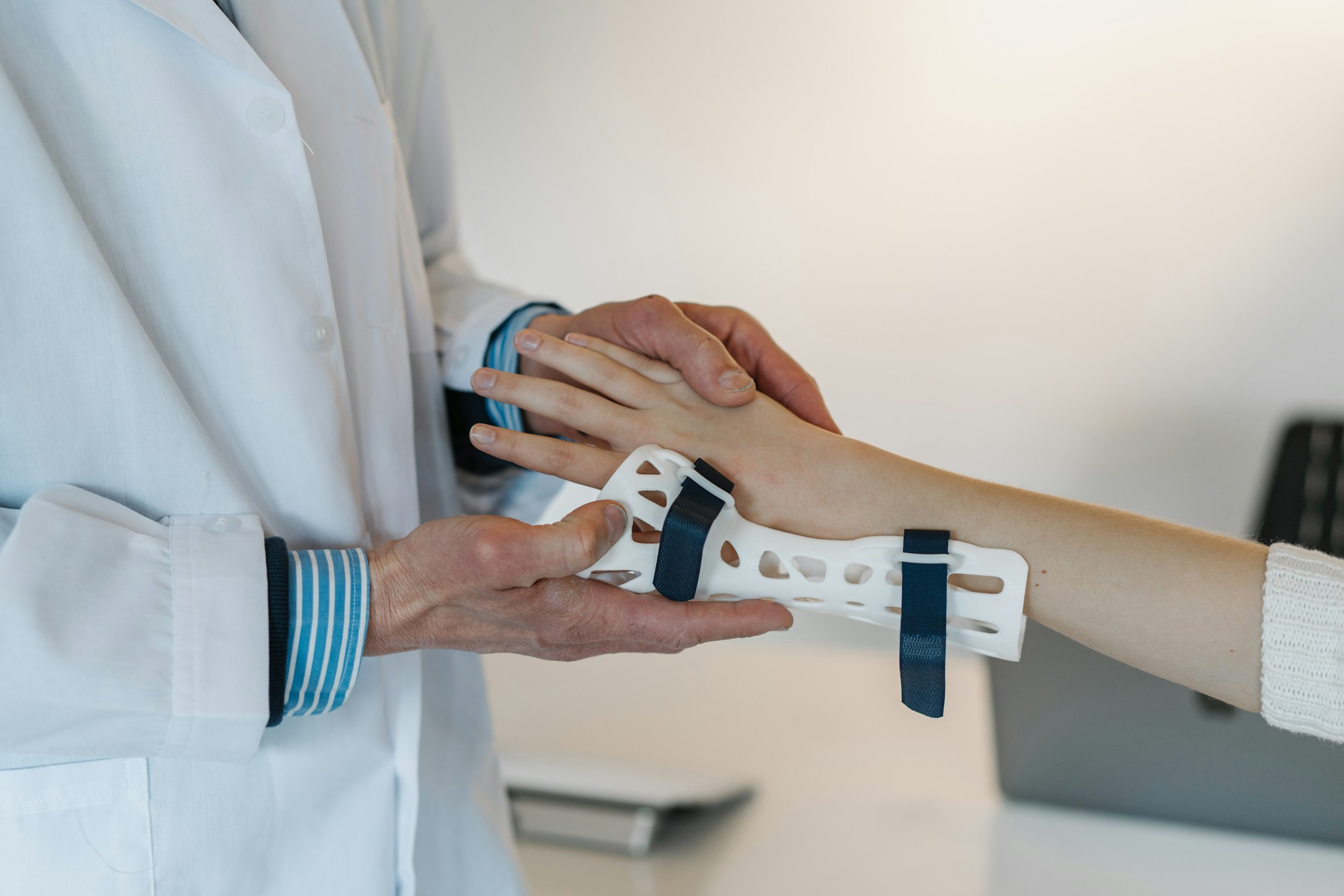
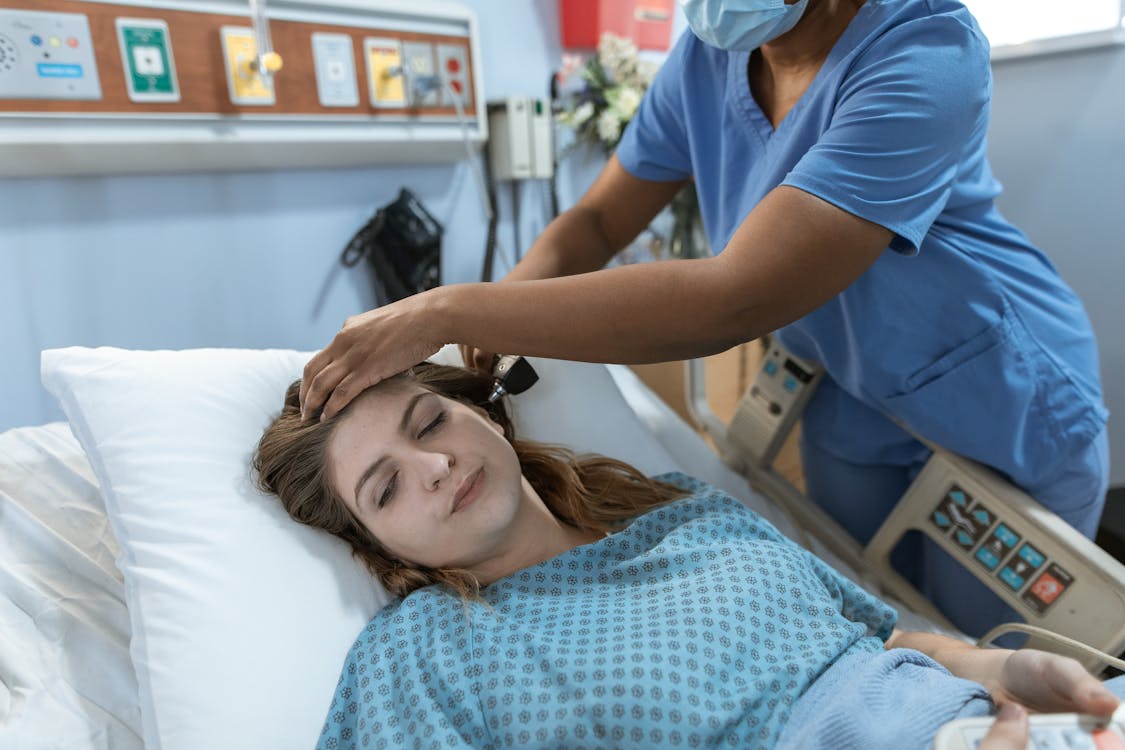
Close of COVID-19 Might Convey Important Turbulence for U.S. Healthcare – JEMS: EMS, Emergency Health care Companies


By RICARDO ALONSO-ZALDIVAR Linked Push
WASHINGTON (AP) — When the close of the COVID-19 pandemic will come, it could build major disruptions for a cumbersome U.S. health and fitness treatment process produced a lot more generous, adaptable and up-to-day technologically through a raft of temporary unexpected emergency actions.
Winding down those people procedures could start as early as the summer time. That could pressure an believed 15 million Medicaid recipients to locate new resources of coverage, involve congressional motion to preserve broad telehealth access for Medicare enrollees, and scramble particular COVID-19 guidelines and payment policies for hospitals, medical professionals and insurers. There are also thoughts about how crisis use approvals for COVID-19 remedies will be managed.
The array of problems is tied to the coronavirus public health and fitness crisis very first declared more than two years in the past and periodically renewed given that then. It’s set to conclude April 16 and the expectation is that the Biden administration will prolong it by mid-July. Some would like a for a longer period off-ramp.
Linked: What Does the Upcoming Maintain for EMS just after COVID-19?
Transitions do not bode perfectly for the advanced U.S. health treatment process, with its mix of non-public and authorities insurance policies and its labyrinth of insurance policies and techniques. Overall health care chaos, if it breaks out, could create midterm election headaches for Democrats and Republicans alike.
“The flexibilities granted through the public health unexpected emergency have assisted people today keep protected and get obtain to care, so shifting ahead the important issue is how to build on what has been a results and not shed ground,” said Juliette Cubanski, a Medicare skilled with the nonpartisan Kaiser Spouse and children Basis, who has been looking into prospective effects of winding down the pandemic emergency.
MEDICAID CHURN
Medicaid, the condition-federal wellbeing insurance policies system for lower-cash flow men and women, is masking about 79 million people, a file partly because of to the pandemic.
But the nonpartisan City Institute believe tank estimates that about 15 million folks could reduce Medicaid when the general public overall health emergency finishes, at a level of at least 1 million for each thirty day period.
Congress amplified federal Medicaid payments to states because of COVID-19, but it also essential states to preserve men and women on the rolls during the wellbeing unexpected emergency. In normal occasions states routinely disenroll Medicaid recipients whose incomes rise further than specified ranges, or for other daily life adjustments affecting eligibility. That process will change on yet again when the emergency ends, and some states are keen to transfer forward.
Almost all of people getting rid of Medicaid are predicted to be eligible for some other supply of protection, either by means of employers, the Affordable Treatment Act or — for young children — the Children’s Overall health Insurance coverage Software.
But that is not heading to come about instantly, said Matthew Buettgens, lead researcher on the City Institute study. Cost and deficiency of consciousness about alternatives could get in the way.
People dropped from Medicaid may perhaps not recognize they can select up taxpayer-backed ACA coverage. Medicaid is ordinarily free, so folks offered workplace coverage could uncover the premiums far too significant.
“This is an unparalleled situation,” claimed Buettgens. “The uncertainty is genuine.”
The federal Facilities for Medicare and Medicaid Companies, or CMS, is advising states to choose it slow and link Medicaid recipients who are disenrolled with other potential coverage. The company will preserve an eye on states’ accuracy in generating eligibility decisions. Biden officials want coverage shifts, not losses.
“We are centered creating sure we keep on to the gains in protection we have built below the Biden-Harris administration,” explained CMS Administrator Chiquita Brooks-LaSure. “We are at the strongest position in our historical past and we are likely make absolutely sure that we keep on to the protection gains.”
ACA coverage — or “Obamacare” — is an choice for many who would get rid of Medicaid. But it will be significantly less reasonably priced if congressional Democrats are unsuccessful to increase generous economic help known as for in President Joe Biden’s social legislation. Democrats stalling the bill would deal with blame.
Republicans in mainly Southern states that have refused to grow Medicaid are also vulnerable. In individuals states, it can be really difficult for low-cash flow grownups to get coverage and additional folks could wind up uninsured.
Point out Medicaid officers don’t want to be the scapegoats. “Medicaid has completed its occupation,” said Matt Salo, head of the Countrywide Association of Medicaid Administrators. “We have looked out for actual physical, mental and behavioral wellness desires. As we occur out of this emergency, we are intended to suitable-measurement the program.”
TELEHEALTH STATIC
Millions of People in america uncovered telehealth in 2020 when coronavirus shutdowns led to the suspension of routine health-related consultations. In-human being visits are once more the norm, but telehealth has revealed its usefulness and acquired broader acceptance.
The end of the public wellbeing crisis would jeopardize telehealth access for hundreds of thousands enrolled in conventional Medicare. Restrictions predating COVID-19 restrict telehealth predominantly to rural citizens, in element to mitigate versus wellbeing care fraud. Congress has specified itself 151 times immediately after the conclude of the general public well being emergency to arrive up with new principles.
“If there are no alterations to the law right after that, most Medicare beneficiaries will drop obtain to protection for telehealth,” the Kaiser Foundation’s Cubanski said.
A significant exception applies to enrollees in personal Medicare Advantage programs, which commonly do protect telehealth. However, almost 6 in 10 Medicare enrollees are in the standard payment-for-company program.
Exams, VACCINES, Remedies, PAYMENTS & Techniques
Widespread entry to COVID-19 vaccines, exams and treatment options rests on lawful authority linked to the general public well being unexpected emergency.
One particular case in point is the Biden administration’s need for insurers to cover up to 8 no cost at-household COVID-19 tests per month.
An region that’s especially murky is what occurs to assessments, therapies and vaccines coated underneath crisis use authorization from the Foods and Drug Administration.
Some authorities say emergency use approvals past only as a result of the period of the general public wellness crisis. Other individuals say it’s not as easy as that, because a distinct federal crisis statute also applies to vaccines, checks and treatment options. There is no very clear route yet from wellbeing officers.
The Fda has granted whole approval to Pfizer-BioNTech’s COVID-19 vaccine for individuals 16 and more mature and Moderna’s for those people 18 and more mature, so their continued use would not be influenced.
But hospitals could consider a monetary hit. Now they’re paid 20% a lot more for the treatment of COVID-19 people. That additional payment is only for the length of the emergency.
And Medicare enrollees would have more hoops to jump by to be authorised for rehab in a nursing residence. A suspended Medicare rule necessitating a prior 3-working day medical center remain would arrive back into influence.
Overall health and Human Solutions Secretary Xavier Becerra not too long ago advised The Linked Press that his office is committed to offering “ample notice” when it finishes the general public health crisis.
“We want to make guaranteed we’re not placing in a harmful situation Americans who however will need our help,” Becerra reported. “The a person that persons are definitely anxious about is Medicaid.”